A while back a post went up after a talk on difficult airways which featured a range of characters and the rolling of a few dice. Well with a revisit for a small group session with clever ED types, the post is updated here. Now, you can still look at the other version here if you want to do a compare and contrast. But there are updates and extra bits here, so maybe just lodge here. And get ready to roll.
The aim of this thing is very simple: to cover all there could possibly be to know about the difficult paediatric airway in a very short bit. Or not, of course. If it was that easy to cover a lot of the subspecialty of paediatric anaesthesia wouldn’t really be a thing.
What can be done in a little short bit is a revisit of things most of us know because sometimes the important thing is to take up some time and space to look at things slightly differently.
So let’s go on a quest. A quest to conquer the airway version of a dragon – rare and a bit scary. I guess this makes me the Quest Master (look, I’d go with Dungeon Master but there would probably be some sort of copyright issue there, I don’t know).
Of course any quest needs heroes which means we need to introduce some characters.
The Characters
Each character hopefully brings some special skills to the table. They are, in no particular order:
The Engineer – who is good with their hands and getting practical stuff done.
The Master Toolsmith – skilled in the acquisition and selection of things that are required.
The Philosopher – the philosopher is particularly good at thinking and thinking about thinking.
The Butcher – good with a knife and OK with the sight of blood.
Oh, and there will be one other character who will only appear as an evil, disembodied laugh in your consciousness. But more of that later.
And Now The Quest …
The local health facility in The Village, which actually services almost all the kids needing serious care locally, is going through challenging times. Forced underground by extensive renovation and rebuilding works to “facilitate better health experiences” and left short-staffed by unanticipated entirely predictable surges in demand, it draws on people who had wholly different lives before they started working in the emergency department. An engineer, a master of tools, a philosopher and a butcher.
While on a break and bonding over war stories and some non-alcoholic mead the heroes are approached by the triage nurse. A 2-year-old patient with a background of trisomy 21 has arrived and they’ve ingested caustic material which probably had nothing to do with the cafeteria. The triage nurse asks the team to assess and manage the patient, making sure to utter trigger words relevant to the scenario,
“He’s heading for a tube.”
The First Question
The first question I had as QuestMasterTM was “which airway in the emergency department should we think of as difficult?”
For this particular day, the answer was very prompt – every episode of airway management in the emergency department is difficult. Which was really convenient because the answer I’d prepared was “we should assume every airway in the emergency department is difficult”.
Not that long ago Long, Sabato and Babl published work looking at the intubations across a year in a busy (and I’m sure, very good) paediatric emergency department. With all their 82,000 presentations per year they needed to perform a total of 71 intubations. There were adverse events in 39%. The first pass intubation success rate was 78% and their first pass success without desaturation or hypotension was 49%.
Kids’ airways are tough for experienced kids emergency practitioners.
That said it is worth taking the time to take note of particular things that might make it tough. Obviously the respiratory and cardiovascular status are important considerations as are any underlying conditions known to be associated with difficult airway management (syndromes and neuromuscular things are a good starting point) because most kids’ difficult airways are predictably difficult, not a complete shock.
And slowing down to make a point of examining the airway can help. Even in kids I still quite like the LEMON mnemonic (for Look, Evaluate, Mouth Opening, Obstructions (like swelling, saliva, blood, fractures, foreign bodies or masses etc) and Neck (movement and anatomy) as long as you take note of the fact that Evaluation with things like thyromental distance isn’t that easy to remember in kids (but size of jaw, position of thyroid/larynx and the like are worth having a look at) and mouth opening can be hard to assess (but is more useful than Mallampati which should formally include tongue protrusion).
Assessment is really valuable, and all these things (plus the obvious ones like kids 2 and under (particularly 1 and under) and smaller as well as all the syndromes that immediately make you think ‘airway’ are worth noting.
The key point though, as discussed with the aid of The Philosopher on this particular day, is that treating all airways in ED as difficult makes sense because the real world evidence suggests that good ED teams find them difficult. Plus if you set up like the situation is going to be difficult, you’re ahead of the game for the greater number of times when it’s not.
Quests are boring if you allow too much latitude of course. So for now, lets condense all the clever talk into something that is very often right – the triage nurse was correct.
Let’s Pause Time
Now in any good quest there is usually scope for the use of special items. For this quest the first special item, represented in the form of a large clock, the team was allowed to deploy the “FirstNet Magical Device of Time Relativity” capable of making time speed up, slow down or become entirely unhinged from reality in the manner of all good computer systems.
So our heroes took the step (after some very intense hinting) of suspending time so they could go and check the old books, in particular “The Book of Ye Olde Knowledge and Understandings” to make sure that some simple things about the paediatric airway and its management were understood equally by all.
So we wanted to double check that the things we all knew about blades, rings and cuffs was up to date.
Except the problem with old books is they need updating, and sometimes the best bits are the helpful scrawls in the margins where people have provided newer info.

What do the marginalia have to say?
Well we now know that it’s not so vital whether or not you choose a straight laryngoscope blade or a curved blade in kids, it’s about using the right technique. We know that the cricoid ring quite possibly isn’t the narrowest part of the paediatric airway. We know that, used appropriately, a cuffed endotracheal tube is usually a perfectly reasonable option. (And because this site has covered that stuff before, you can go here for more details or even here.)
[Quick sidenote on the cricoid ring thing which has been covered on the site plenty of times before. There has been an interesting interjection recently in the form of this review article where they compare a bunch of autopsy studies extending waaaay back to the in vivo work that suggests that it’s not the cricoid that’s the narrowest bit. They side with the idea that the autopsy studies are more accurate and clinically relevant because the in vivo studies are done in patients who have had their airway influenced by decreased muscle tone with anaesthesia, or functional movement of the airway that happens when you’re alive or other changes you observe in patients who are alive.
This is a particularly interesting take because it seems to amount to “you should pay more attention to the studies that were in autopsy specimens, because they are free of all of the clinical changes that actually relate to the patients you look after”. I am unconvinced. Either way the broader point might just be that it is most important to safely use of endotracheal tubes by appropriately choosing sizes and monitoring cuff pressure.]
We still had some time thanks to the FirstNet Magical Device of Time Relativity so we took the opportunity to drop by the armoury to gather the tools we’d need for the job, a task undertaken by the Master Toolsmith.
The Armoury
Again there was a lot of good discussion about what to choose and how to think about what you’d need. Broadly the Master Toolsmith made sure there was the requisite equipment to undertake pre-oxygenation and basic airway management, the necessary equipment for plan A (being intubation with a laryngoscope (video or direct) and an appropriate endotracheal tube and one size down), suction, those things necessary to secure the airway so the applied option didn’t fall out, the necessary drugs for the intubation and after intubation care and the things you’d want for the other potential plans (supraglottic airways and surgical options).
The Set-Up
With kit in hand the heroes also moved straight onto talking about how they’d set up to get it done. In brief there are probably 4 things to think through, and really you could spend plenty of time mocking up layouts and the like:
- The space – think about the layout of your working space. How much access do you have around the treatment area? Are the things you need logically laid outing easy to get to? Are the things you need right now closest to you? Is there anything you can optimise?
- The bed – I mention this one specifically because so often people seem to be stuck on the idea that the bed must be absolutely flat for airway instrumentation. Why? Have a really good think about whether having the patient sitting up at least a little might be a better option for functional residual capacity and respiratory management.
- The kit – you’ve chosen it but have you double checked it worked and briefed what you’ll do.
- The people – the agreement of most seemed to be that you’d probably want four people ideally. One to manage the drugs, one for doing the technical stuff, one as the assistant and one keeping an eye on the big picture. Of course if you’ve trained for it you can do it with less but we’re talking about optimising things where we’ve assumed a difficult airway.
We spent just a little time in this small session discussing the importance of considering calling for expert back-up when managing the airway and the idea of setting limits in advance for what would make you call for that back-up.
Of course if they’d tried to use some sort of “Charmed Summoning Rock of the Switch”, or even a “Demon Brick Screen of Auditory Person Grabbing” that would not have served the quest particularly well so it’s just as well they didn’t try.
Oh, and one quick note on the drugs. Both the talk and post version are waaaay too brief to go through all the ins and outs of choosing induction agents but perhaps the crucial bit is to get comfortable with a couple of agents and be familiar both with the advantages of said drug and the things that aren’t so desirable that can happen with that potion.
The members of the crew had some really interesting comments on this, particularly in variance between places they’d worked. Some had previously worked in departments where propofol was routinely used and therefore felt comfortable with this option (at least at the time they were regularly using it). One person had previously used plenty of ketofol and one had more experience with ketamine. All could cite pros and cons of different options and that’s sort of the key point – there is no drug free of side-effects and in a tricky situation that familiarity with an agent is pretty important. There’s no need to add another element of stress when there’s a chance you’re feeling a little stressed.
Zen
Now this might be a fake medievalist quest but the good people of this village know the benefit of a few moments of quiet meditation. And that’s what preoxygenation is good for. The key elements of pre oxygenation appear to be successful delivery of high concentrations and time.
It’s also important to note that applying nasal prongs to sit under the mask isn’t necessarily going to help preoxygenation. It doesn’t seem to enhance the expired oxygen levels after a few minutes of preoxygenation. This is probably because in adding those prongs you break the seal for a mask which allows entrainment of 21% oxygen and violates the “deliver high oxygen concentrations” bit. In fact in some of the controlled testing, the only patient group who do better with nasal prongs in place are the ones where you deliberately create a break in the seal.
The mainstay of preoxygenation should still be a mask that fits well with a circuit delivering high-flow oxygen and time (think at least 3 minutes). The basics done superbly.
The 3 minutes of zen time also lets you talk through what you’ll do and take a few deep breaths yourself.
Also, as extensively covered here, the addition of THRIVE probably does extend apnoeic time and keeping those saturations up is certainly likely to make you less stressed and is a noble thing to strive for anyway. However, once you’re extended beyond a few minutes it doesn’t remove the need to progress through an airway plan to achieve your primary goals. You can’t just push on forever.
What about DSI and kids? Well there’s not an overwhelming amount of evidence for it, particularly in kids. There’s the original series described by Weingart et al. and then there’s a few cases described in kids. Anecdotally I’m aware of plenty of people who use an approach of sub-anaesthetic dosing of ketamine in particular to achieve the goal of good preoxygenation. It’s a reasonable approach to achieve a goal and one of those occasions where the adult stuff seems to extrapolate to kids pretty well.
Oh, and the other thing of course is that if you go down the RSI route the modern modifications to that include face-mask ventilation (in a gentle fashion) and a real priority on maintaining oxygenation (but more of that here).
Let’s Roll the Dice
As for any good quest, we need something to help us know if the chosen path leads to success or not. Which is where these come in …
The Engineer, being the person to get practical things done picked up the 20-sided dice and rolled an 19. Which happily was a very good number to roll (although anything over 3 would have done the job because more often than not things will go fine). The preoxygenation was brilliant, the medications were well chosen, the laryngoscopy was not at all an issue and the endotracheal tube was placed without any fuss at all.
Success! \o/
Of course at that moment, our fifth player enters in the form of an ominous and evil laugh…
This is of course The Evil Necromancer of the Executive Suite who, armed only with a clipboard and an email account, is capable of inflicting multiple contradictory realities on hardworking clinicians at any moment.
So just as our heroes have triumphed, they find themselves back at the point of preoxygenation, ready to roll again.
Roll 2
The dodecahedron is rolled this time and the number 9 comes up. Or maybe it wasn’t 9. But it was definitely a very disappointing number to roll. The attempt at intubation is unsuccessful.
So at this point, what things are going through the mind (apart from ‘which idiot who recently watched “Stranger Things” again based an airway talk on a Dungeons and Dragons game…)?
Well most departments will have something like the following on the wall and will have trained to work through it…

Now this is a good algorithm with lots of sensible things on it. It’s also one that might be hard to work through in the heat of battle with an airway dragon. It’s one to have tried to digest beforehand.
I checked with The Philosopher (and actually the whole crew felt like this) who agreed that at times of stress it’s pretty useful to be able to reduce our thinking to simple things. Things that we can visualise easily and know what they mean.
I personally quite like the simple mental overlay offered by the Vortex Approach.
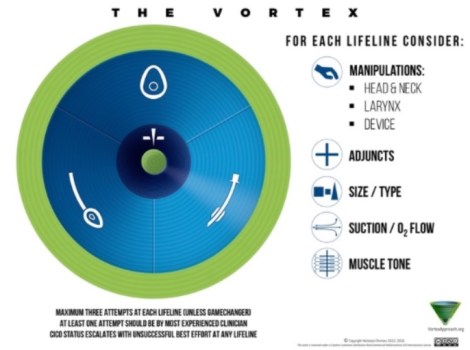
It’s just a good reminder that there are three things to try optimising and stresses the need to keep moving (appropriately) and with caution.
All the details behind it are probably beyond inclusion here so maybe go and have a look at the site and see what you think.
Whichever mental pathway they used to get there, let’s say The Engineer asked the Master Toolsmith for a supraglottic airway and they reached a point of safety with successful oxygenation. \o/
Success!
But then the evil laugh of The Evil Necromancer of the Executive Suite rang out again.
The team are back at the point where preoxygenation was just ending…
The Third, Fourth and Fifth Rolls…
This time all the rolls for mask, supraglottic airway and endotracheal tube came up with the wrong number. Look, it doesn’t matter which wrong number they were all just the wrong number.
The time came for a player who had offered many words but not many actions to step forward. It was time for The Butcher.
At this point in the artificial scenario it was time to chat through different front of neck access techniques. Actually even before the it was time to mention that CICO situations in kids are really super rare. At the institution I work at I think there’s been a single episode in the operating theatres in 20+ years.
You can also look at stuff from the PeDI airway registry, a specific multi-institution study looking at difficult airway cases. It’s defined in that study as including kids who have difficult laryngeal exposure (think Cormack and Lehane 3+), those in whom conventional direct laryngoscopy is impossible, children with prior failed direct laryngoscopy within 6 months, and in those where alternate techniques were chosen.
In that super difficult group thee was a total of around 2% of patients (of their 1018) who had some form of surgical airway. The other thing that matters though is that there were only 10 recorded cases where either face-mask ventilation or supraglottic insertion were impossible (and it’s hard to get a sense of whether there was overlap in those groups).
So the chances of truly failing oxygenation seem incredibly low, and if the planning has been done and support summoned then the chances of ending up at this part of the algorithm in the ED really seems incredibly low.
Still, preparedness matters in any village health facility.
The most important things to note about front of neck access in kids would be:
- The suggested techniques in different age groups are based on consensus and that consensus is invariably hard for people to arrive at. Most people seem to suggest cannula cricothyroidotomy in the under 8s, but I’ve seen some paediatric anaesthetists publish opinions that those kids should definitely have a scalpel technique deployed. Either way the anatomy can be hard to define and there are those who suggest abandoning all pretext of finding the cricothyroid membrane and just aim for trachea. Access to the area can also be difficult just because it’s a tight little spot. Any which way in smaller kids the trachea is very pliable and it is very easy to produce posterior tracheal wall injury or even puncture. There are no good options here.
- The best bet is therefore not getting to that point.
The best review of recent times on this topic is by that punter Sabato again (and was discussed here on this website).
As a general point on this if you are looking at front of neck access there are a few practice points worth contemplating:
- It’s worth continuing to attempt to provide oxygen from the top end.
- Prepare early – briefing it before everything is a good start and after that first challenging attempt ideally someone should be starting to get ready with just that job in mind.
- That person has to mentally focus only on managing access from the neck.
- After that it’s important to slow things down a little rather than try to be super fast, talk out loud through what you’re doing and involve the team. You might as well share that stress.
Amazingly in this case the Butcher deploys a cannula with excellent technique, hooks up to an appropriate device for provision of oxygen without jetting ginormous pressures and achieves oxygenation just as those summoned by that pesky magic rock turn up.
Success! \o/
And this time The Evil Necromancer must be on a conference call because there is only silence.
Coda
The patient and their airway have been successfully managed. The team will retell their story, first to the other workers who will take over care of the patient and then in the parchment version of the patient record so others may hear tales of their noble quest.
They will recall that all paediatric airways could be considered difficult. They will write new books in which the useful things in the marginalia are actually just the things written in the books. They will teach people about knowing their equipment and set-up, briefing a well-drilled team, optimising their chances with each technique and the great joy to be found within the meditation of pre-oxygenation. They will talk about achieving clarity through simpler thinking at moments of stress.
And at the end of the shift they might just go and find some mead that isn’t labelled non-alcoholic. And even plan their next encounter with a different kind of dragon.
Notes:
This version has some of the clever stuff from the small group in here. I’ve obscured their IDs because I didn’t double check in advance whether they’d mind if I mentioned they were clever. They know who they are and maybe I’ll get to update with their details.
The paper by Long, Sabato and Baby on the experience of intubation at RCH ED in Melbourne is here:
You can find the post that covers myths in paeds airways here.
A colleague from CareFlight, Dr Chris Groombridge, did a nifty little study in pre oxygenation and the best expired oxygen achieved here:
And there’s a similar one showing that having those high-flow nasal prongs probably only makes pre-oxygenation better where you don’t have a seal with the mask.
The Weingart DSI thing is this one:
Interested in the Vortex Approach and didn’t click up there above? Try out here.
Want to look at the paeds difficult intubation registry thing? Then try this:
Here’s the Sabato and Long review on CICO in kids:
And here’s the paper on the development of difficult paeds airway guidelines:
Did you get all the way to the end here? Well good on you and have a reward. I know you’ve seen it already but it’s epic so let’s go with something that’s a little like a dragon. Enjoy this baby iguana escaping snakes over and over and use it as a metaphor for something in your daily life. That’s right I didn’t even update this bit because I like it so much.

Pingback: Different Dragons – A Quest Updated | Prehospital and Retrieval Medicine - THE PHARM dedicated to the memory of Dr John Hinds·
Dear Andrew, what device do you use to vacuum pack your pre-packed airway gear in the difficult airway trolley? Thomas ________________________________
LikeLike
Hi Thomas. It’s literally a Foodsaver vacuum packing for food thing. I’m sure any food-sealingdevice thing would do the job.
LikeLike
Pingback: The 2018 Year in Review | Songs or Stories·